TRACHEOTOMY
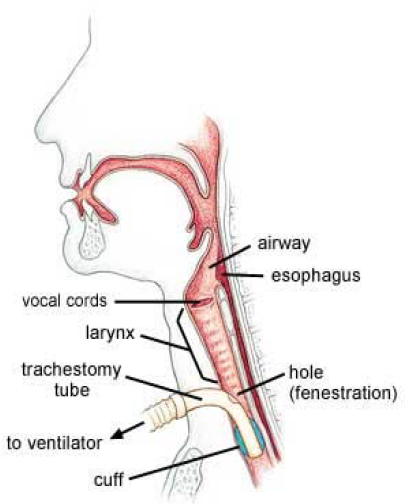 Tracheotomy is a procedure in which a tube (typically an inert plastic or silicone tube) is surgically inserted through an incision in the low part of the neck, into an opening created in the trachea (windpipe) below the level of the larynx (voice box). There are many different reasons that patients may undergo tracheotomy (trach). Often, the reason is because of the need for prolonged mechanical ventilation (respirator), replacing the endotracheal tube already present in the patient. Sometimes it is performed to bypass obstruction of the upper airway due to scar or tumor or vocal cord paralysis. Other indications are for treatment of severe obstructive sleep apnea, or improving the ability to manage secretions in a patient who is chronically aspirating (choking on their own saliva).
Tracheotomy is a procedure in which a tube (typically an inert plastic or silicone tube) is surgically inserted through an incision in the low part of the neck, into an opening created in the trachea (windpipe) below the level of the larynx (voice box). There are many different reasons that patients may undergo tracheotomy (trach). Often, the reason is because of the need for prolonged mechanical ventilation (respirator), replacing the endotracheal tube already present in the patient. Sometimes it is performed to bypass obstruction of the upper airway due to scar or tumor or vocal cord paralysis. Other indications are for treatment of severe obstructive sleep apnea, or improving the ability to manage secretions in a patient who is chronically aspirating (choking on their own saliva).
Tracheotomy surgery is done in the hospital. It is typical for the patient to remain hospitalized for about one week after the procedure. Sometimes, depending on the reason for the tracheotomy, the patient might then be transferred to a long-term ventilator hospital / rehab / nursing home. On other occasions, if the patient is competent to care for the tracheotomy on his/her own, he/she may be discharged home after appropriate education has been provided and necessary supplies have been arranged in the home. Just because someone has had a tracheotomy placed, it does not mean it will be there permanently. The length of time that one needs to keep the trach tube is entirely dependent on the reason that it was placed. For instance, if the tube is placed for assistance with ventilator support, and patient’s cardiopulmonary status improves so that the ventilator is no longer necessary, then it may be possible to remove the trach tube. The process for removing a trach tube, called decannulation, may take anywhere from a few days to a few months. In other instances, if the trach tube has been placed because of an irreversible neurological condition, it is likely that it will remain in place for the duration of the patient’s lifetime. Each individual circumstance is different.
There will be lifestyle changes once a tracheotomy tube is placed. As an example, water must be kept away from the trach tube because the water could be inhaled (aspirated). This means a patient with a trach tube should not swim. There are also issues that arise with speaking when a patient has a tracheotomy. Most often, there is at least an initial period of time right after the surgery when there will be no ability to speak. This lets the wounds heal. In general, as long as a patient needs to be on a ventilator, speaking will typically not be possible. Once the patient no longer requires a ventilator, consideration might be given for speaking.
Eating may be possible with a trach, again depending on the reason the tracheostomy tube was placed. For instance, if the trach is for severe obstructive sleep apnea, a special plug is placed into the trach tube during the daytime, and only opened at night. These patients can generally eat normally and have nearly normal daily activities. On the other hand, if a trach tube is placed for airway protection because of a stroke or other neurologic disease that causes difficulty swallowing, it is unlikely that this type of patient will be able to eat or drink by mouth, irrespective of a trach. These patients often require feeding tubes to maintain nutrition.
The indications and risks of surgery, as well as expected outcomes, must be understood prior to proceeding with your surgery. In addition, you must understand your alternatives to the surgery. The alternative is not to have the surgery performed, and continue with medical management of the problem. This would leave you/the patient in the current condition.
SURGICAL RISKS/COMPLICATIONS
BLEEDING: Minor bleeding from the incision is typically not a problem; however, heavy bleeding deeper in the neck can be very serious and can potentially cause difficulty with breathing. Rarely, a return to the operating room is necessary.
WOUND INFECTION: Infection after tracheotomy is uncommon. If this was to develop this is managed with local wound care and other medicines as needed. 3) PNEUMOTHORAX (COLLAPSED LUNG): The tracheotomy is performed just above the top of the lungs. It is exceedingly rare to injure the lungs, but to be sure this complication hasn’t occurred, a chest x‐ray is ordered just after the surgery. If a pneumothorax was to occur, another procedure would need to be performed to re‐expand the lung.
AIRWAY SCARRING: This is fortunately very rare, but a serious complication of any airway surgery. Indeed, even the presence of an endotracheal tube (often the tube that we are replacing by tracheotomy) can cause airway scarring. One of the reasons to convert an endotracheal tube to a tracheotomy is to minimize the risk of airway scarring. The scarring can be at the level of the vocal cords, below the level of the vocal cords (subglottic stenosis), or in the trachea itself (tracheal stenosis). If this was to occur, depending on the level of the scar formation, often further surgery or surgeries are necessary to improve this condition. Airway scarring might lead to the need for a permanent trach tube.
TRACH TUBE DISLODGEMENT: Fortunately this is rare, but if it occurs it can be devastating and/or fatal. This most often occurs if the ‘trach ties’ around the neck are kept too loose allowing for the tube to become displaced out of the airway. This problem is best avoided by paying close attention to the appropriate ‘snugness’ of the ties.
As with any type of surgery, the risks of anesthesia such as drug reaction, breathing difficulties and even death are possible. Please discuss these risks with your anesthesiologist. Fortunately, with this procedure, anesthetic problems are exceedingly rare.
At Suburban Ear, Nose and Throat Associates, Ltd., we go to great lengths to try to help you understand your plan of care. If at any time during your care you have questions or concerns, please call us at 847‐259‐ 2530.
