
Submandibular Gland Excision
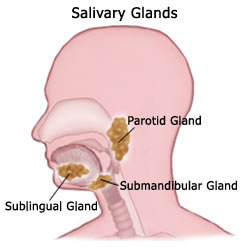
The three major salivary glands in the head and neck are the parotid, submandibular, and sublingual glands (see above diagram). In addition to these major glands, there are over 500 minor salivary glands lining the inside of the mouth. Thus, if one gland is surgically removed, you will not likely notice any degree of dry mouth. Saliva lubricates the mouth to aid in swallowing, and also decreases bacterial overgrowth, which can lead to tooth decay.
Tumors may also arise from the salivary glands. Salivary gland tumors may be benign (non-cancerous) or malignant (cancerous). Surgical removal is the main treatment for tumors of the salivary gland. A fine needle aspiration (FNA) biopsy can be done under local anesthesia, either in the office or hospital, to help with the diagnosis. If the tumor is malignant, radiation and/or chemotherapy may be used in conjunction with surgery.
When it comes to the submandibular gland, surgery is usually recommended or recurrent infections of the gland (sialoadenitis), which have failed medical management. Sometimes, infections are caused by recurrent salivary stones (sialolithiasis). However, as stated above, surgery may also be recommended to address both benign and malignant disorders of the salivary gland.
How does a problem with the submandibular gland present?
Sometimes people present with a mass or lump in the neck. Usually, imaging such as CT scan will localize that the mass is involving the submandibular gland. You also might have intermittent swelling with or without pain in the area of the gland. This may or may not be due to stones that cause obstruction to salivary flow, which can create chronic infections or swelling.
What does surgery involve?
The gland will be removed via an incision in a crease of your neck below your jaw line. The gland must be dissected away from surrounding muscles, blood vessels and nerves. General anesthesia is used for surgery. Some patients go home the same day, but most will stay overnight. In most cases, a small drain will be placed in the wound. After surgery, the patient will probably have some discomfort and pain medicine is usually prescribed. It may or may not be necessary to remove stitches. If those need to be removed, it is usually done a week after surgery. The patient may shower or have a sponge bath at home one to two days after surgery, after the drain is removed. Recovery takes about 1-2 weeks. A follow-up appointment about 1-2 weeks after the surgery is typically made to check how the area is healing.
Two Weeks Before Surgery: Avoid all non-steroidal anti-inflammatory drugs (“NSAIDs”), including aspirin, ibuprofen, Motrin, Advil, Naproxen and others, because these medications may increase bleeding. You may be instructed to stop multivitamins. Please discontinue homeopathic or alternative medicines, such as ginseng or ginkgo biloba as these may also increase bleeding.
Day Before Surgery: You may eat a regular diet and take most of your medicines the day before surgery, but nothing is to be eaten after midnight. Clear liquids (water, tea, Gatorade) can be taken up to four hours before surgery. If taking medicines, please check with your physician to see which should be continued.
Hospital Stay: Excision of the submandibular gland may require an overnight hospital stay.
Lab Work: Your physician may request that bloodwork is done prior to surgery. If this is needed, you will receive an order form for this bloodwork, and the location of the lab to perform the blood draw is usually recommended based on your insurance company and where your surgery is to be performed.
After Surgery: Usually there is no restriction on what you can eat or drink after surgery. A drain may be placed in your neck after surgery. We request that aspirin and NSAIDs should not be taken for 2 weeks after surgery due to increased risk of bleeding. We recommend avoiding strenuous activity for 2 weeks after surgery to minimize the risk of bleeding or fluid collection in the neck.
The indications and risks of surgery should be understood prior to proceeding with surgery. You should understand the alternatives to the surgery. Your alternative includes not having the surgery performed, which would leave you in your current condition. If you have chronic infections, you could continue with intermittent antibiotic treatment. If you have salivary stones, sometimes these stones are amenable to direct excision through the mouth, but not in all cases.
SURGICAL RISKS AND POSSIBLE COMPLICATIONS:
Despite the fact that surgery in the neck involves dissection in proximity to many important structures such as vessels and nerves, excising this salivary gland is usually performed without difficulty or long-term complications. Most patients usually leave the hospital the day of or the day after surgery.
After any surgery, some pain is normal, but if it does not decrease or worsens, it may be abnormal and indicate infection or bleeding. Bleeding and infection are possible, as with any surgery. There is not a high incidence of either of these complications with this type of surgery. The drain that may be placed during surgery is designed to help prevent these. You may get bruising of the neck around the incision.
There will be a scar, which will be carefully planned and sewn. Usually the scar from this type of surgery blends well into natural neck creases, but sometimes patients can get thickening or excess scar tissue such as hypertrophic scar or keloid. If the scar heals with unsatisfactory appearance, scar revision is possible. There is often numbness of the skin around the incision, which will recover slowly as the small sensory nerves supplying the skin heal.
Rarely, a collection of saliva can form after surgery called a sialocele, which may require repeated drainage. If this tracks to the skin, a fistula may develop which may require further surgery or treatment. If a salivary stone is left behind, this may require further surgery if it causes infections.
There are 3 important nerves located near the submandibular gland. ‘Bruising’ of these nerves can occur causing temporary weakness. Long-term or permanent weakness to these nerves is rare. These risks may be increased when there is malignancy or history of many infections in the gland. Damage to the marginal mandibular branch of the facial nerve can cause weakness of your lower lip muscle causing a crooked smile. The lingual nerve supplies sensation to the tongue, and damage would cause numbness of the tongue. The hypoglossal nerve allows the tongue to move, and if weak it can cause difficulty with tongue motion.
The operation is carried out under general anesthesia. As with any type of surgery, the risks of anesthesia such as drug reaction, breathing difficulties, and even death are possible. Please feel free to discuss any specific concerns about anesthesia with the anesthesiology team.
GENERAL POST-OPERATIVE INSTRUCTIONS/CARE
Activity: Light activity (lifting)
Diet: General diet as tolerated is recommended.
Medicines: Pain medications are typically prescribed. These are to be taken as directed. Antibiotics may also be prescribed.
Bathing: Generally, showering is fine 24 hours after the surgery after the drains are removed. No bathing or soaking in water is recommended until after the incision is healed.
Post-operative follow-up: Sutures may be dissolvable or may have to be removed a week after surgery. A post-operative follow-up is typically scheduled for about a week after surgery, but may be needed sooner if you leave the hospital with a surgical drain in place.
At Suburban Ear, Nose and Throat Associates, Ltd., we go to great lengths to try to help you understand your plan of care. If at any time during your care you have questions or concerns, please call us at 847‐259‐2530.
- Submandibular Gland Excision


